Dry Drowning: An Update
Our series of articles on dry drowning have elicited lots of interest and feedback from readers, which is great. As a reminder, here are the three previous articles:
- Dry Drowning, by Walt Bammann – Walt started us off with his report.
- Dry Drowning Feedback
- Dry Drowning Revisited
Walt appears to have experienced a laryngospasm, an involuntary muscular contraction of the vocal cords in the throat. This effectively blocks the airway and prevents air, and therefore oxygen, from getting to the lungs.
There is some public confusion around the term dry drowning. We’re not medical professionals, so we’ll leave the technical distinctions between dry drowning and laryngospasm to those professionals. What we’ll concern ourselves with here is if you cannot breathe after (usually) being tossed in the water unexpectedly.
Since we ran the most recent article, Dry Drowning Revisited, we’ve received several good responses from readers that deal with the phenomenon and how to recover from it. We thought it was time for a dry drowning update, so here is their feedback:
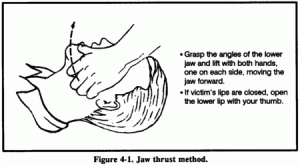
“I read your article regarding ‘dry drowning’ with interest from the perspective of a kayaker and a health care professional in the field of anesthesia. On occasion, patients we care for in the operating room suffer from laryngospasm and require intervention to prevent further complications. As you say, getting help is important, but most often direct treatment must promptly ensue. First, the jaw thrust maneuver, which many Wilderness First Responders and all EMT’s should know, usually ‘breaks’ a laryngospasm. The next step is, as you suggest, mouth to mouth breathing, which imparts positive air pressure on the closed airway and hopefully opens it. These two interventions may be done simultaneously for improved chances of success. There is an art to mouth-to-mouth breathing (no pun intended), which has the possibility of inflating the stomach leading to regurgitation and further problems if not done correctly.
“Thanks for your continued whitewater safety publications and tips for those of us trying to have a safe, memorable time on the river!”
Joshua Mackie, CRNA
“I had a laryngospasm incident when I was in the US Marine Corps doing some preparatory training for attending scuba diving school in 1994. As a young, fit, very strong swimmer, it was surprising to me that a small splash of water landing at the right place in my windpipe, during a “bobbing” activity in the deep end of a swimming pool, would trigger a complete blockage due to this reflex, but that is what happened. Fortunately, I was in a fairly well-controlled environment and a safety diver was able to quickly bring me to the side of the pool. Without belaboring all the details of the training exercise, the gear I was wearing made me negatively buoyant and without help it was a major effort simply to break the surface of the water to attempt to breathe…you can only manage to try this a few times before you are sufficiently oxygen deprived and begin to gravitate toward the bottom of the pool. Another fortunate circumstance was that the Navy corpsman that was providing pool-side emergency medical support was formerly a Navy SEAL; he saw what happened to me and had seen this before with other experienced swimmers. He taught me that the trick to surviving this type of spasm is actually quite simple, but completely non-intuitive and against all instincts one would have in this situation.
“Here it is: simply arch your head back, way back, as if someone was positioning your airway to start rescue breathing…this will force open the musculature under spasm and you will again be able to breathe. (Editor’s Note: This is essentially replicating the “jaw thrust” that Joshua recommends above.)
“I wish this simple technique was widely publicized to swimmers, boaters, and particularly scuba divers. I suspect the many “strong swimmers” who drown do not start the process as panicked individuals who then transition to asphyxiation due to laryngospasm or suddenly start inhaling water…I believe it is the spasm that causes the panic and sets the process in motion.
“Scenario-type 1: If the person can keep additional water from hitting the area near the windpipe, and “relax” in an air-rich environment, the spasm may resolve within 30-60 seconds. This appears to be the “lucky” scenario of Walt Bammann.
“Scenario-type 2: In many situations it will be necessary to both reach a source of air and tilt the head way back to overcome the spasm…waiting for the muscles to “relax” is untenable before loss of consciousness ensues (note that having your airway completely blocked causes more than a little distress).
“Examples of scenario-type 2 situations where air is available, but the person is unable stop the spasm because copious amounts of water are in or near the airway occurs in scuba diving, swimming or boating in rough water, and situations where one person is trying to rescue someone else in the water.
“A couple of years after I learned the tilt-your head-way-back trick it saved me while I was scuba diving near an oil rig in the Gulf of Mexico. I was about 100 feet under the surface swimming around the rig structure, as I swam upside down to circle under a crossbeam, the diaphragm in my regulator got momentarily stuck such that I inhaled some seawater…the body did its part by closing off the windpipe…I was a bit startled, but not panicked, I grabbed my second regulator, tilted my head way back to open the airway, tilted my head and coughed a bit, then started breathing normally.
“Earlier today a colleague at work mentioned that he just got back from the funeral of another employee’s 15-year old son who drowned at a nearby lake. The teenager was a strong swimmer and was swimming from a boat to the shore. The distance couldn’t have been more than a quarter mile. He hadn’t been drinking. Did he encounter a laryngospasm? If so, the tilt-your-head-back-way-back technique could have saved him.
“I plan to publish a paper on this topic soon to try and raise awareness. Please share this simple technique with the swimmers, boaters, and divers you know.”
Jeff Brewer
“I believe that I experienced laryngospasm in May last year after my first flip during training. The water was so cold and I was scared and could not breathe. Another guide in my boat (a paramedic) could tell that I could not breathe and she told me to exhale. Because of the cold water and the unexpected swim I had taken a huge gulp of air and could not breathe until I let it out. It did not feel like I could exhale, but exhaling forced relaxation which also helped me breathe. Having an action such as exhaling rather than just being told to relax is very helpful when relaxing is the last thing that you are able to do. This was the scariest thing I have ever experienced but the solution was very simple. I am so glad that you are educating people on what to do. Exhaling is the best solution I have ever seen.”
Amy Cooper
“Laryngospasm (or laryngeal spasm) can be initiated by a number of things, one of which is water contacting the larynx. If this occurs, and the airway is completely blocked for long enough, the victim will suffocate.
“A far more likely consequence of immersion, however, particularly in cold and/or rough water, is near drowning, a well-documented, frequent, and particularly insidious consequence of aspirating water. Near drowning can be fatal long after the person is out of the water. For this reason, anyone who has aspirated more than a tiny amount of water would be wise to seek immediate medical attention.
“Incidentally, there’s some debate about the role of laryngospasm in dry drownings and the term itself is not synonymous with dry drowning.
“With respect to cold water drownings, it’s worth noting that the primary danger associated with cold shock is immediate and total loss of respiratory (breathing) control which dramatically increases the potential for water aspiration and sudden drowning.”
Moulton Avery
“Laryngospasm (aka Dry Drowning) Is covered by the ABCDE method taught in Wilderness and Remote First Aid and also in the Lifeguard Professional Rescuer Manual:”
Caring for Respiratory Distress
You do not need to know the cause of respiratory distress to provide care. When you find a victim experiencing difficulty breathing, activate the emergency action plan (EAP) and:
- Maintain an open airway.
- Summon emergency medical services (EMS) personnel.
- Help the victim to rest in a comfortable position that makes breathing easier.
- Reassure and comfort the victim.
- Assist the victim with any of his or her prescribed medication.
- Keep the victim from getting chilled or overheated.
- Administer emergency oxygen, if available and you are trained to do so.
Someone with asthma or emphysema who is in respiratory distress may try to do pursed-lip breathing. To assist with this, have the person assume a position of comfort. After he or she inhales, have the person slowly exhale through the lips, pursed as though blowing out candles. This creates back pressure, which can help to open airways slightly until EMS personnel arrive and take over.
“This could also be an ASTHMA attack so that is a good reason to know what medical conditions exist for the paddlers on a trip or outing. For those with asthma; do you carry your EMERGENCY inhaler in your PFD?”
Kurt, a sea kayaker
Good stuff – thanks to all of you!
Let’s summarize the above input and that from the previous articles:
- Dry drowning, or laryngospasm, does occur – often enough that we should all be aware of it.
- Some 10-15% of “drowning” victims have little or no water in the lungs. If a swimmer is having this problem and is unable to reach shore or get help they run the risk of becoming part of that 10-15% statistic.
- When someone goes for a swim, all other party members need to quickly locate the swimmer(s) and check on them. A person experiencing a laryngospasm is likely to be disoriented and quite possibly panicky. And, they will be having a problem requesting help.
- One great boating signal that everyone should learn is the “are you okay?” signal. The rescuer shouts or whistles to get the swimmer’s attention and then pats the top of their head. The swimmer, if they think things are under control, replies by patting the top of their head. This works well when distance and/or noise make verbal communication difficult. Always include the description of this signal in your pre-trip safety talk.
- When suffering from a laryngospasm, the swimmer needs to do their best to get the attention of others. The universal “I’m choking” signal is grasping the throat with both hands. In turbulent water, this might not be seen or could be misinterpreted as keeping the life jacket from riding up. The boater signal for “things are not okay, or stop” is arms held up and forearms crossed. This will be very visible. When rescuers draw close, the hands to the throat is great non-verbal communication.
- When Walt got to shore he was able to breathe, and for some, just being encouraged to relax can relieve the spasm. Quite possibly just being connected with rescuers will let a swimmer relax enough to start breathing.
- Performing the jaw thrust or simply tilting the head far back can relax the muscles and open the airway. And possibly trying to exhale can also have a positive result. If not, a mouth-to-mouth rescue breath will likely unlock the larynx. This can be performed while the swimmer is still in the water.
- This is unlikely to happen to any one of us, but it will happen to some of us. Advance knowledge of the phenomenon can go a long way toward helping both swimmers and rescuers respond quickly and correctly. Pass the word along to people you boat with.
- Anyone experiencing this phenomenon will be wise to get a medical exam as soon as they can. Having the airway blocked and struggling to breathe can create a partial vacuum that draws fluid from the body into the lungs. This can cause additional delayed medical issues.
And speaking of passing the word along to your fellow boaters, here’s a good example of positive action taken:
“On Saturday, I tried whitewater rafting for the first time and had exactly the experience described by Walt Bammann in his article. It took me three days to do the right Google search, but I am so happy to have found it. I actually felt embarrassed and wondered if I was overreacting, or making up the seriousness and scariness of the experience.
“All I could think about was getting my breath, and I couldn’t grab the paddle extended to me, or the rescue rope. I remember thinking, oh the guy behind can get that… Getting my hand onto the loop at the end of the rescue kayak felt like a super human effort. As soon as I was in a raft and out of the water, the problem resolved almost immediately and I could breathe, but I had purple lips for 15 minutes after I was deposited on land (one of the other rafters kept exclaiming about it until it got better).
“I will be emailing the owner at the rafting centre. Although their rescue system worked fine, it’s clear that they didn’t realize what had happened and I am keen to spread the word (the irony of this being that I am a huge talker!!).”
Elizabeth Currie
Elizabeth is doing her bit to spread the word about laryngospasm-related boating incidents. Please do the same in passing this info along to other boaters. The life you save can be a friend or loved one… or your own.
Boat Often and Boat Safe,
—Clyde
e-News Editor
 NRS Gift Card: Always Fits, Always Wanted
NRS Gift Card: Always Fits, Always Wanted




